Staphylococcus aureus
Staphylococcus aureus is not only one of the most important human bacterial pathogens resulting in considerable morbidity and mortality, but also is a common member of the skin microbiota. Persistently colonizing the skin of roughly one third of U.S. adults, S. aureus is the leading cause of skin, soft tissue, and surgical site infections. Colonization is a risk factor for localized epithelial infections, which can allow bacteria to gain access to deeper tissue, resulting in invasive disease such as endocarditis, osteomyelitis, sepsis, and severe pneumonia. Further, the widespread prevalence of S. aureus strains resistant to methicillin and all beta-lactam antibiotics (MRSA) found in both hospitals and communities presents an escalating threat to human health worldwide. Addressing the critical knowledge gap of how S. aureus persists in and breaches the skin epithelia has potential to deliver tremendous preventative and therapeutic value.
S. aureus possesses an impressive arsenal of virulence factors, many of which have been studied in the context of disease. However, considering that S. aureus colonizes the keratinized epithelia of many individuals asymptomatically, we hypothesize that S. aureus virulence factors also play important roles in modifying the skin to facilitate bacterial colonization. To explore S. aureus interactions with host epithelial cells, we employ in vitro infection assays with human keratinocytes, an ex vivo 3D human organotypic epidermal culture model, and a variety of murine models of S. aureus infection.
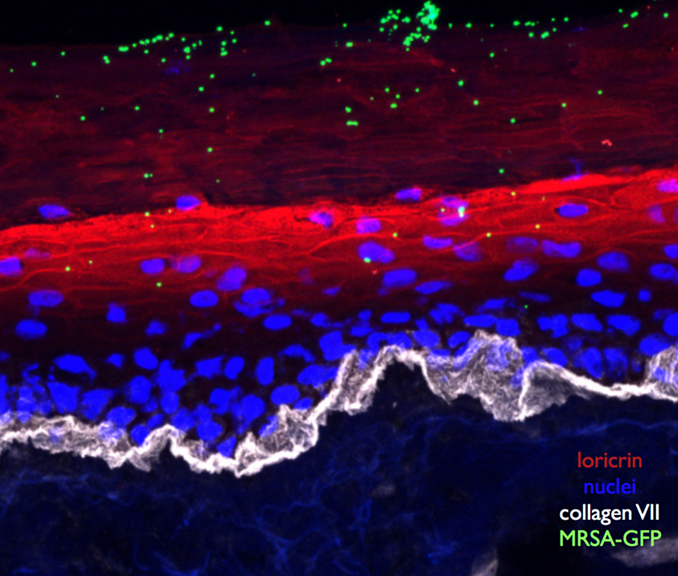
Cross-section of a fully differentiated 3D human organotypic epidermal tissue infected with MRSA-GFP. Collagen VII is present at the interface between the dermis and epidermis. Loricrin localizes to the granular layer and the squames of the stratum corneum. Bacteria are seen growing into microcolonies on the surface and between squames in the stratum corneum. Image credit: Lauren Popov.
Current S. aureus projects in the lab seek to address the following questions:
How does S. aureus use virulence factors to modify the host skin epithelia during colonization and disease?
How does S. aureus manipulate the epithelial junctions to facilitate bacterial colonization?
How do host cellular junctions modulate disease outcomes of S. aureus epithelial infections?
Staphylococcus aureus is not only one of the most important human bacterial pathogens resulting in considerable morbidity and mortality, but also is a common member of the skin microbiota. Persistently colonizing the skin of roughly one third of U.S. adults, S. aureus is the leading cause of skin, soft tissue, and surgical site infections. Colonization is a risk factor for localized epithelial infections, which can allow bacteria to gain access to deeper tissue, resulting in invasive disease such as endocarditis, osteomyelitis, sepsis, and severe pneumonia. Further, the widespread prevalence of S. aureus strains resistant to methicillin and all beta-lactam antibiotics (MRSA) found in both hospitals and communities presents an escalating threat to human health worldwide. Addressing the critical knowledge gap of how S. aureus persists in and breaches the skin epithelia has potential to deliver tremendous preventative and therapeutic value.
S. aureus possesses an impressive arsenal of virulence factors, many of which have been studied in the context of disease. However, considering that S. aureus colonizes the keratinized epithelia of many individuals asymptomatically, we hypothesize that S. aureus virulence factors also play important roles in modifying the skin to facilitate bacterial colonization. To explore S. aureus interactions with host epithelial cells, we employ in vitro infection assays with human keratinocytes, an ex vivo 3D human organotypic epidermal culture model, and a variety of murine models of S. aureus infection.

Cross-section of a fully differentiated 3D human organotypic epidermal tissue infected with MRSA-GFP. Collagen VII is present at the interface between the dermis and epidermis. Loricrin localizes to the granular layer and the squames of the stratum corneum. Bacteria are seen growing into microcolonies on the surface and between squames in the stratum corneum. Image credit: Lauren Popov.
Current S. aureus projects in the lab seek to address the following questions:
How does S. aureus use virulence factors to modify the host skin epithelia during colonization and disease?
How does S. aureus manipulate the epithelial junctions to facilitate bacterial colonization?
How do host cellular junctions modulate disease outcomes of S. aureus epithelial infections?